Program Search
Programs to Fit Your Lifestyle & Goals
Discover hundreds of flexible continuing education options, tailored for working professionals seeking certifications or university coursework to achieve their goals.

Actuarial Exam Preparation
-
Type
Credit Certificate -
Format
Hybrid -
Semester
Fall, Spring, Summer
UVM’s Pre-Actuarial Certificate is for students with strong math skills and an undergraduate degree who want to pass the Actuarial Science certification exams and work as an actuary.

Agroecology, Food Sovereignty and Social Movements
-
Type
University Coursework -
Format
Online -
Semester
Fall, Spring
Available as a non-credit, 14-week online course, students will investigate the social, political, and economic elements of the global food system from multiple perspectives.

Artisan Cheese & Sensory Fundamentals Professional Certificate
-
Type
Certificate -
Format
Online -
Semester
Fall, Spring
A foundational 4-week online program for cheese enthusiasts, food systems professionals, cheesemongers, and aspiring cheesemakers.

Building Healthy Brains
-
Type
University Coursework -
Format
Online -
Semester
Fall, Spring, Summer
At the University of Vermont, we have developed an in-depth understanding of the unique challenges faced by those who provide services to transition-age youth (TAY).

Cannabis Plant Biology Professional Certificate
-
Type
Certificate -
Format
Online -
Semester
Fall, Spring
Created in UVM’s College of Agriculture and Life Sciences, this 8-week, fully online, and evidence-based program will cover cannabis chemicals, genetics, agricultural best practices, post-harvest handling, and processing, and how cannabis affects the human body through an examination of basic pharmacology and the different modes of administration.

Cannabis Science and Medicine Professional Certificate
-
Type
Certificate -
Format
Online -
Semester
Fall, Spring
Offered through The Robert Larner, M.D. College of Medicine at The University of Vermont Department of Pharmacology, UVM is the first medical school in the nation to offer a professional certificate in cannabis and medicine for therapeutic use, providing you with a competitive advantage as a knowledgeable and trustworthy provider. UVM’s 8-week, fully online program covers cannabis history, business, law and policy, plant biology, biological effects on humans, production and safety, pharmacology, and clinical research.

Career Pathways into Teaching
-
Type
Graduate Program -
Format
Hybrid -
Semester
Fall, Spring, Summer
UVM’s nationally recognized and accredited graduate programs offer you a flexible, high-quality pathway into a teaching career.

Certificate in Cybersecurity
-
Type
Credit Certificate -
Format
Online -
Semester
Summer
UVM’s certificate in Cybersecurity is designed to develop a comprehensive foundation in the knowledge and skills necessary for a career in cybersecurity.

Certificate in Gerontology
-
Type
Credit Certificate -
Format
Hybrid -
Semester
Fall, Spring
Challenge misconceptions about aging and replace them with information firmly grounded in reality.

Certificate of Graduate Study in Agroecology
-
Type
Credit Certificate -
Format
Hybrid -
Semester
Fall, Spring, Summer
Composed of one hybrid course, three foundational online courses, and final synthesis online seminar course, the goal of the CGSA is to provide participants with graduate-level, conceptual, and applied knowledge in agroecology.

Certificate of Graduate Study in Complex Systems and Data Science
-
Type
Credit Certificate, Graduate Program -
Format
Online -
Semester
Fall, Spring
Gain data science expertise with the Certificate Graduate Study in Complex Systems and Data Science at the University of Vermont. Learn wrangling, visualization, machine learning techniques, and more to uncover stories underlying complex systems.

Certificate of Graduate Study in Education for Sustainability
-
Type
Credit Certificate -
Format
Hybrid -
Semester
Fall, Spring, Summer
Empower your students by earning an Education for Sustainability Certificate from UVM, a program designed to help educators accelerate positive change in their school and community.
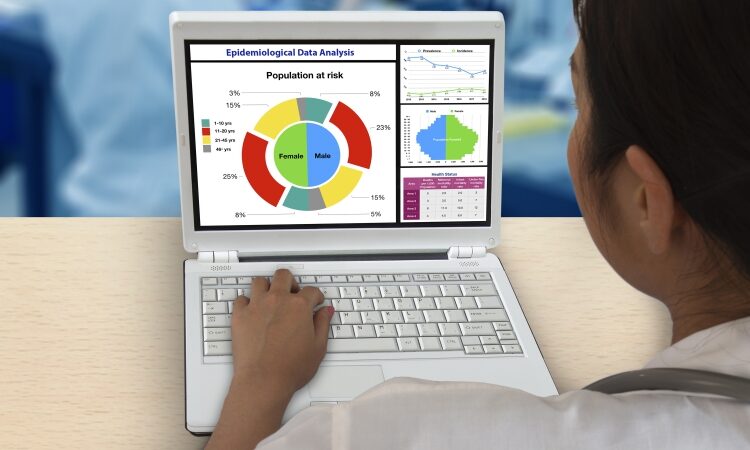
Certificate of Graduate Study in Epidemiology
-
Type
Credit Certificate, Graduate Program -
Format
Online -
Semester
Fall, Spring
UVM’s Certificate of Graduate Study in Epidemiology provides students with a framework for problem-solving and critical thinking in analyzing disease and health-related conditions within diverse populations.

Certificate of Graduate Study in Global and Environmental Health
-
Type
Credit Certificate, Graduate Program -
Format
Online -
Semester
Fall, Spring
Develop expertise in a range of health hazards, health-promotion strategies, and environmental public health practices with this one-year Certificate of Graduate Study in Global and Environmental Health.

Certificate of Graduate Study in Healthcare Management and Policy
-
Type
Credit Certificate, Graduate Program -
Format
Online -
Semester
Fall, Spring
Explore policy, finance, and management issues impacting healthcare and public health with this one-year Certificate of Graduate Study in Healthcare Management and Policy.

Certificate of Graduate Study in Public Health
-
Type
Credit Certificate, Graduate Program -
Format
Online -
Semester
Fall, Spring
Build a strong foundation in population health sciences, including epidemiology, biostatistics, and environmental health with this Certificate of Graduate Study in Public Health.

Certificate of Graduate Study in Sustainable Enterprise
-
Type
Credit Certificate, Graduate Program -
Format
Online -
Semester
Fall, Spring, Summer
Discover the power of the triple bottom line sustainability framework in your business strategy and drive competitiveness while championing sustainability.

Companion Animal End-of-Life Doula Professional Certificate
-
Type
Certificate -
Format
Online -
Semester
Fall, Spring, Summer
When a beloved animal is nearing end-of-life, stress can be high. Enter UVM’s End-of-Life Doula program specializing in companion animals.

Compassionate Leadership
-
Type
Certificate -
Format
Online -
Semester
Fall, Spring
Participants will cover topics of leadership, career development, productivity, selling, and personal empowerment.

Computer Software Certificate
-
Type
Credit Certificate -
Format
Hybrid -
Semester
Fall, Spring, Summer, Winter
Advance your career in an IT-related field, earn credits toward a computer science degree, or take the first step to become a software developer.

Credit Courses
-
Type
University Coursework -
Format
On Campus, Online, Hybrid -
Semester
Fall, Spring, Summer, Winter
Refresh your knowledge, learn a new skill, pursue a passion, or prepare for an advanced degree with courses at UVM. Explore hundreds of options from American Sign Language to Creative Writing, Human Biology, Public Health, and more. Chart your path today.

Digital Marketing Fundamentals Professional Certificate
-
Type
Certificate -
Format
Online -
Semester
Fall, Spring
This fully online certificate offers students with minimal or no prior digital marketing experience the opportunity to gain a comprehensive overview of digital marketing and establish themselves as a digital marketing expert.

Ecological Economics Graduate Certificate
-
Type
Credit Certificate, Graduate Program -
Format
On Campus -
Semester
Fall, Spring, Summer
Learn a framework for solving humanity’s environmental challenges by analyzing the interdependence of the economy and the environment.

Ecological Foundations of Agroecology
-
Type
University Coursework -
Format
Online -
Semester
Fall, Spring
Available as a non-credit, standalone offering, this 15-week, online course, examines the ecological foundations of Agroecology, largely from a biophysical perspective.

Education and Social Services Professional Development Courses
-
Type
Certificate -
Format
On Campus, Online -
Semester
Fall, Spring, Summer, Winter
We prioritize teaching, research, and services that are student-centered, family-focused, community-engaged, and culturally competent.

Emotional Intelligence and Leadership
-
Type
Certificate -
Format
Online -
Semester
Fall, Spring
Participants will actively apply the intentional change theory and work through its stages to develop their own emotional competencies and improve their leadership effectiveness.

End-of-Life Doula Professional Certificate
-
Type
Certificate -
Format
Online -
Semester
Fall, Spring, Summer, Winter
UVM’s online End-of-Life Doula Professional Certificate prepares students for the increasing demand for end-of-life support. Start your end-of-life doula training today.

Farmer Training Program
-
Type
Certificate -
Format
On Campus -
Semester
Summer
UVM’s Farmer Training Program is a six-month, hands-on program for aspiring farmers and food-systems advocates that provides experiential, skills-based education in sustainable farming. Students will get a unique and comprehensive education by running all aspects of the 10-acre Catamount Educational Farm, learning from expert farmers and educators in the classroom, and alongside successful, inspiring farmers in the Burlington area.

Food Systems Graduate Program
-
Type
Graduate Program -
Format
On Campus, Online -
Semester
Fall
Combining knowledge with action, UVM’s 18-month, transdisciplinary, cohort educational model program prepares students to apply knowledge of the interconnected and interdependent global food system and helps them develop skills in mixed method research approaches in order to critically analyze and propose solutions to our most challenging problems.

Geographic Information Systems and Data Communication Professional Certificate
-
Type
Certificate -
Format
Online -
Semester
Fall, Spring, Summer, Winter
Discover why UVM is a leader in training and certification in geospatial technologies with our GIS certificate program. Develop your skills for data-driven decision-making today!

Integrative Health and Wellness Coaching Program
-
Type
Certificate, Credit Certificate -
Format
On Campus, Online -
Semester
Fall, Spring
Help people make healthy lifestyle changes with our health and wellness coaching programs. UVM’s program meets the requirements for national board certification.

Integrative Healthcare Certificate
-
Type
Credit Certificate -
Format
Hybrid -
Semester
Fall, Spring, Summer
UVM’s Integrative Healthcare Certificate prepares students to understand traditional methods of healthcare with complementary care and self-care. Start your integrative health certificate today.

Intro to Data Analytics & Intro to Python for Data Analytics
-
Type
Certificate -
Format
Online -
Semester
Fall
Earn career-boosting credentials in UVM’s Data Analytics Certificate Program. Gain the technical skills and experience you need to build data models, create data visualizations, and make data-driven business and technical decisions.

Introduction to Agroecology
-
Type
University Coursework -
Format
Online -
Semester
Fall, Spring, Summer
Available as a non-credit, standalone offering, this 4-week, online course presents an in-depth overview of research and applications in the field of agroecology, with a focus on principles-based approaches.

Just Transitions – Food Systems
-
Type
University Coursework -
Format
Online -
Semester
Spring
Available as a non-credit, standalone online offering. Students will explore how agroecological transitions are complex, relational and ongoing processes of change that unfold in territories, and shaped by these wider processes within a complex matrix of power.

Leading Effective Teams
-
Type
Certificate -
Format
Online -
Semester
Fall, Spring, Summer
Participants will learn the key sources of motivation for empowered teams and how team leaders must account for the special and unique circumstances of working in a team, where responsibility, accountability, communication, and leadership are shared.

Legal Issues in Higher Education Conference
-
Type
Conference -
Format
On Campus, Online -
Semester
Fall
The University of Vermont annually presents one of the nation’s premier legal conferences.
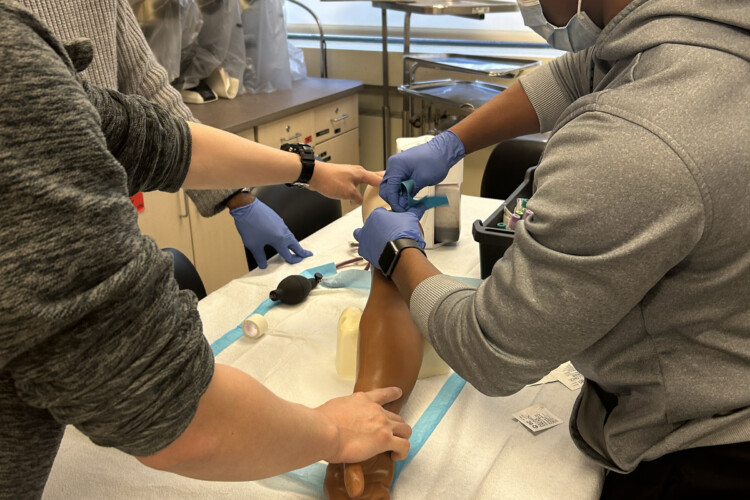
Master of Medical Science Degree
-
Type
Graduate Program -
Format
On Campus, Online -
Semester
Fall, Summer
Pursue your dream of medical school with UVM’s Master of Medical Science degree. Our program prepares you to make a strong impression on medical or other health-professional schools.

Master of Professional Studies, Leadership for Sustainability
-
Type
Graduate Program -
Format
Hybrid -
Semester
Fall, Spring, Summer
Cultivate leadership practices that prioritize well-being, reciprocity, and relationships while challenging oppression and dominance.

Master of Public Health
-
Type
Graduate Program -
Format
Online -
Semester
Fall, Spring, Summer
Earn your Master’s in Public Health at UVM and promote more just, evidence-based health interventions for diverse populations.

Master of Science in Medical Laboratory Science
-
Type
Graduate Program -
Format
On Campus -
Semester
Fall
Complete the coursework required to be eligible for the American Society for Clinical Pathology certification exam and start your career in diagnostic medicine.

MCAT Prep for UVM Students
-
Type
University Coursework -
Format
Online -
Semester
Fall, Spring, Summer, Winter
UVM and Kaplan have teamed up to provide students with an opportunity to save money and excel on the revised MCAT.

MedCerts Clinical HealthCare Certifications
-
Type
Certificate -
Format
Online -
Semester
Fall, Spring, Summer
Increase your earning potential and find rewarding work in one of the fastest-growing industries in the U.S. — healthcare through online training on-demand.

MindEdge at UVM
-
Type
Certificate -
Format
Online -
Semester
Fall, Spring, Summer
UVM Professional and Continuing Education offers a variety of self-paced online courses through a partnership with education innovator MindEdge, Inc.

Osher Lifelong Learning Institute (OLLI)
-
Type
Workshop -
Format
On Campus, Online -
Semester
Fall, Spring, Summer
The Osher Lifelong Learning Institute (OLLI) at UVM provides year-round workshops and events that are diverse, interesting, fun, and affordable for a community of adult learners. Explore offerings on campus at UVM, across the state, and online.

Participatory Action Research and Transdisciplinary Agroecology
-
Type
University Coursework -
Format
Online -
Semester
Fall
Available as a non-credit, 14-week, online course, students will have the opportunity to examine examples of agroecological PAR projects, draw upon lessons learned, and find inspiration.

PhD in Food Systems
-
Type
Graduate Program -
Format
Hybrid -
Semester
Fall
When you earn your Ph.D. in Food Systems, you’ll join a cohort that works together to devise potential solutions to society’s biggest challenges within our food system.

Post-Baccalaureate Medical Laboratory Science
-
Type
Credit Certificate -
Format
On Campus -
Semester
Fall, Spring, Summer
With UVM’s medical lab science program, you can get the training you need to be eligible for the American Society for Clinical Pathology certification. Start your career in diagnostic medicine today.

Post-Baccalaureate Pre-Medical Program
-
Type
Credit Certificate -
Format
On Campus -
Semester
Fall, Spring, Summer
UVM’s Post-Bacc Pre-Med program is your solution to realizing your future as a healthcare provider.

Pre-College Courses
-
Type
University Coursework -
Format
On Campus, Online -
Semester
Fall, Spring, Summer, Winter
High school students are invited to take on-campus or online for-credit courses throughout the year with current college students at UVM. Our entry-level courses—ranging from Art History to Wildlife Biology—are appropriate for high school students and UVM’s small class sizes are perfect for interacting with faculty.

Pre-RD Sequence
-
Type
University Coursework -
Format
Hybrid -
Semester
Fall, Spring, Summer
Through UVM, work towards obtaining a Verification Statement and being eligible to apply to internships or a Master’s degree.

Project Management Practices Certificate
-
Type
Certificate -
Format
Online -
Semester
Fall, Spring, Summer
Gain essential project management knowledge and skills – aligned with PMI standards – in just 8 weeks.

Resiliency-based & Trauma-Informed Practices
-
Type
Credit Certificate -
Format
Hybrid -
Semester
Fall, Spring, Summer
UVM offers this coursework to prepare educators and health professionals to address the complex challenges associated with trauma.

School Library Media Specialist
-
Type
Credit Certificate -
Format
Hybrid -
Semester
Fall, Spring, Summer
The University of Vermont offers graduate educational opportunities for those interested in school library media studies to earn licensure in Vermont or to acquire a graduate degree in school library media.

SLP Pre-Master’s Track Program
-
Type
Credit Certificate -
Format
Online -
Semester
Fall, Spring
Offered fully online, UVM’s 19-credit Pre-Master’s speech-language pathologist certificate is designed for students interested in completing the required undergraduate coursework needed to apply to a master’s program.

SLPA Professional Certificate
-
Type
Credit Certificate -
Format
Online -
Semester
Fall, Spring
Get trained and certified with UVM’s SLPA program online. Our program meets all of the American Speech Language Hearing Association’s (ASHA’s) guidelines for the preparation of SLPAs.

Summer Academy
-
Type
University Coursework -
Format
On Campus, Online -
Semester
Summer
UVM’s Summer Academy gives high school students the opportunity to live on campus while taking a college course with other high school students. Students will explore a specific field of study and get a head start on their college career while earning valuable college credits.

TalkVermont
-
Type
Workshop -
Format
On Campus -
Semester
Learn the fundamentals of serious illness conversations and connect more deeply with your patients and their loved ones.
We apologize for not being able to generate any results matching your search criteria. Our professional and continuing education courses, certificates, and graduate programs are constantly updated to ensure they meet the changing needs of our students and the industries they serve. Please try again with new search criteria or contact our support team for assistance in finding the perfect program for you.
